
How Regulatory Compliance Impacts Beauty Clinics
Running a beauty clinic in Canada requires strict adherence to federal and provincial regulations. Compliance ensures safety, legal protection, and trust, while non-compliance risks penalties, reputational harm, and operational disruptions. Health Canada mandates standards under the Food and Drugs Act and Cosmetic Regulations, covering injectables, labelling, and product approvals. Provincial bodies like the CPSO further regulate who can perform treatments and under what conditions.
Key Takeaways:
- Product Compliance: Injectables need a valid Drug Identification Number (DIN), and cosmetics require a Cosmetic Notification Form (CNF) submission within 10 days.
- Labelling Standards: Bilingual labels with specific requirements (e.g., 1.6 mm character height) are mandatory.
- Storage Rules: Neurotoxins and fillers demand cold chain compliance with regular temperature checks.
- Client Consent & Documentation: Poor consent and record-keeping contribute to 30% of complaints against practitioners.
- Verified Suppliers: Using Health Canada-approved distributors ensures safe, compliant products and avoids risks like counterfeit goods.
Compliance is non-negotiable. It protects clinics from legal trouble, maintains client trust, and ensures smooth operations. Non-compliance, however, can lead to fines, lawsuits, and even business closures. By following regulations, clinics can safeguard their reputation and thrive in Canada's growing beauty market.
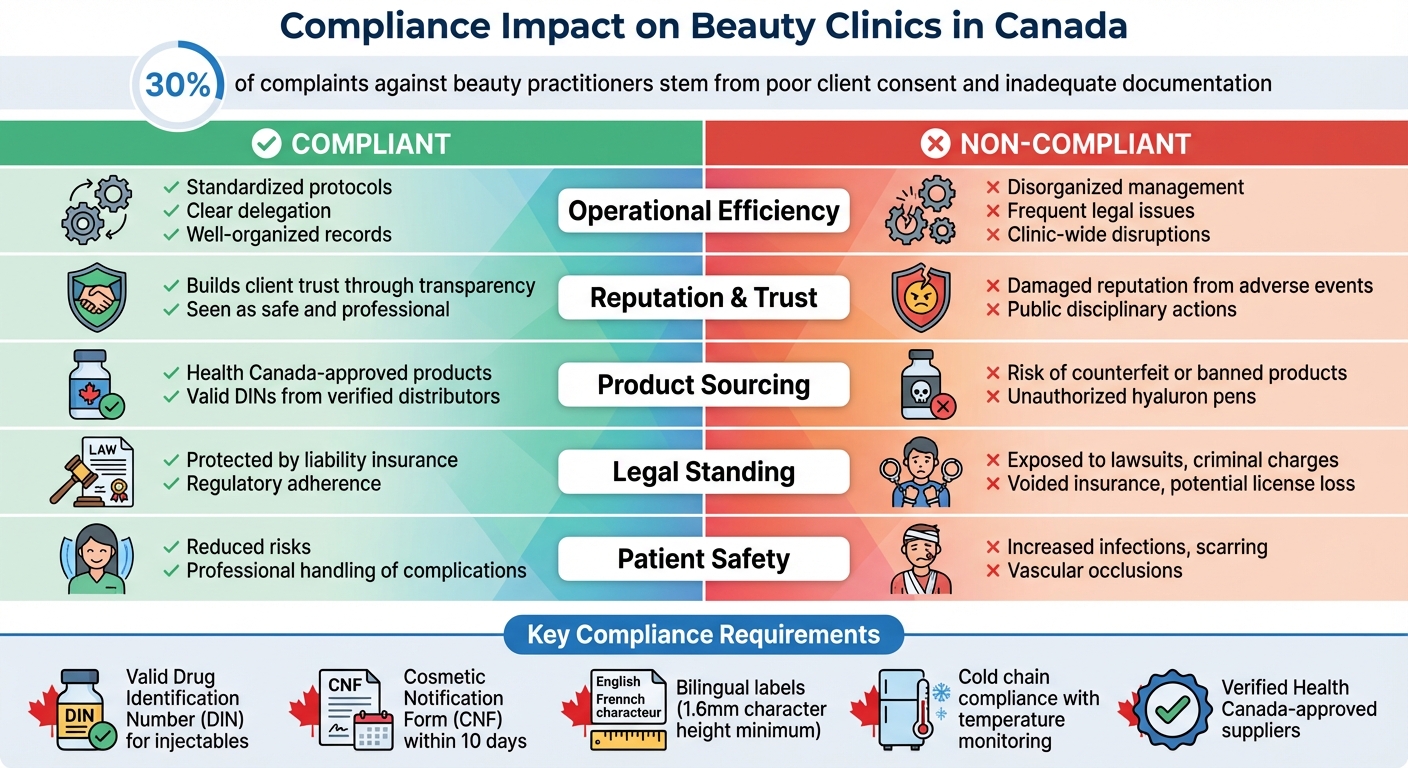
Compliant vs Non-Compliant Beauty Clinics: Operational Impact Comparison
Legal Strategies for Aesthetic Clinics: Compliance, Marketing, and Client Safety
sbb-itb-8ec3e54
How Compliance Affects Daily Operations
Regulatory compliance plays a crucial role in the day-to-day functioning of beauty clinics, influencing everything from product handling to client interactions. It ensures that operations remain smooth and professional, reducing risks and maintaining trust.
Product verification is a cornerstone of these operations. For example, injectables must have a valid DIN, and cosmetic products are required to meet Health Canada's dual-language labelling standards. Labels must also include mandatory information with a character height of at least 1.6 mm for readability. Clinics must meticulously track batch numbers and storage conditions, enabling quick responses to adverse reactions and protecting against potential claims. Interestingly, 30% of complaints against beauty practitioners are linked to poor client consent and inadequate documentation[1]. Efficient product verification lays the groundwork for proper storage management.
When it comes to storage protocols, strict oversight is non-negotiable. Injectables like neurotoxins and dermal fillers demand "cold chain" compliance, meaning medical refrigerators must undergo regular temperature checks to maintain product integrity. In Ontario, these substances fall under controlled acts as outlined in Regulation 107/96. This means that non-prescribing practitioners can only administer them under valid medical directives from a physician or Nurse Practitioner. Additionally, keeping up-to-date client consent and thorough documentation remains a critical part of daily operations.
Adhering to compliance standards not only keeps operations running smoothly but also protects against interruptions. Non-compliance, on the other hand, can result in product recalls, inspections, or even legal trouble. Clinics that follow regulations enjoy efficient workflows and unrestricted market access, while those that don’t face voided insurance coverage and potential lawsuits.
| Operational Area | Compliant Clinic | Non-Compliant Clinic |
|---|---|---|
| Workflow Continuity | Smooth operations with verified products readily available | Disruptions caused by recalls, inspections, or product seizures |
| Legal Risk | Low risk, supported by proper documentation and medical directives | High risk of lawsuits and regulatory penalties |
| Safety Standards | Maintains efficacy with proper storage and aseptic techniques | Increased risk of adverse effects from improper storage or handling |
| Administrative | Accurate record-keeping and adherence to labelling standards | Poor records that could lead to legal disputes |
| Market Reach | Full access across provinces, including Quebec | Limited operations and potential fines under Quebec's Bill 96 |
Reputation: Building Trust vs Facing Penalties
A clinic's reputation thrives on trust. When clients notice you're using products with a valid Drug Identification Number (DIN), it sends a clear message: your clinic prioritizes compliance and safety. This kind of transparency builds credibility, distinguishing professional operations from "under-the-table" alternatives. Leslie Perry, Executive Director of the Professional Beauty Association, highlights this distinction perfectly:
"A license means training, testing and accountability. DIY and under-the-table operators place consumers at risk."
This trust isn’t just about appearances - it directly impacts client loyalty and the overall stability of your business.
On the flip side, non-compliance can have devastating consequences. Take the case of a wellness centre in Alberta in early 2024. They offered "premium Botox" at discounted rates, which initially attracted attention. However, investigators found the Botox lacked Health Canada approval. The fallout? Regulatory scrutiny, negative media coverage, patient distress, and refund demands. But the lasting damage was even worse: a tarnished reputation and a sharp decline in client retention. Incidents like this don’t just bring fines; they leave a permanent stain on a clinic’s public image.
The good news is that transparent practices can rebuild and maintain client confidence. Openly discussing treatment risks, benefits, and alternatives gives clients the power to make informed decisions. This goes beyond a one-time consent form - it's about maintaining an ongoing dialogue. Shannon, a Master Esthetician and Instructor at Reimagine Clinic, stresses the importance of trust:
"The trust your clients place in you is as precious as the treatments you offer. Honour it by protecting their private information and using medical-grade nitrile gloves with the utmost care."
Compliance doesn’t just safeguard your legal standing - it strengthens your reputation, attracts loyal clients, and positions your clinic as a trusted leader in the market. Clinics that prioritise compliance enjoy better client retention, glowing referrals, and even lower insurance premiums. On the other hand, non-compliance brings distrust, lawsuits, and, in extreme cases, business closure. With 30% of complaints against beauty practitioners linked to poor consent practices and documentation, the stakes for maintaining trust and transparency have never been higher.
| Reputational Effect | Immediate Impact | Long-Term Impact |
|---|---|---|
| Client Trust | Confidence in product safety and practitioner expertise | Strong client loyalty and word-of-mouth referrals |
| Legal Standing | Avoidance of fines and regulatory issues | Long-term protection of professional reputation and growth |
| Market Position | Clear differentiation from unlicensed competitors | Establishment as a reliable and respected brand |
| Safety Record | Fewer adverse reactions due to verified products | Reduced insurance costs and a legally secure practice |
Sourcing Supplies: Working with Verified Distributors
The suppliers you choose play a crucial role in maintaining your clinic's compliance with regulations. Verified distributors help ensure that every product aligns with Health Canada's stringent safety standards, covering everything from proper CNF notification to bilingual labelling. This is your clinic's first safeguard against penalties and potential harm to clients.
Take, for instance, the case from January 2026. A practitioner in Kelowna, British Columbia, purchased an "Algae Peel" from an unverified source. The product had a glaring spelling error ("Alage"), lacked an ingredient list, and included no usage instructions. Similarly, a Montreal clinic lost over CA$150 (plus tax) on a Hyaluronic Acid Serum that arrived with a foul odour, making it unusable. These incidents highlight how sourcing from unreliable suppliers can disrupt operations and damage the trust clinics work hard to build. In fact, nearly 47% of beauty sector business owners report financial losses due to supplier errors.
By working with distributors like Beauty Pro Supplies Canada (https://beautyprosupplies.com), you gain access to safe, compliant products and valuable educational resources. These resources cover topics such as selecting injection supplies, understanding advertising claims, and navigating the Cosmetic Ingredient Hotlist. Verified distributors ensure products come with complete INCI ingredient lists, proper documentation, and a Canadian-based Responsible Person for regulatory contact. Health Canada reinforces this point:
"Health-care professionals, including doctors and nurses, must use products that come from reliable sources and meet quality standards." – VIVACY Canada
The difference between verified and unverified sources couldn’t be clearer. Verified distributors provide full traceability and documentation, ensuring your clinic is always audit-ready. On the other hand, unverified sources may deliver products with prohibited substances like mercury or chloroform, incomplete labelling, or missing CNF submissions. These issues can lead to customs seizures, recalls, or fines. With new fragrance allergen disclosure rules coming into effect by April 12, 2026, the margin for error is even smaller. Choosing the right supplier affects more than just compliance - it impacts your clinic’s legal standing, insurance coverage, and client safety.
| Feature | Verified Distributors | Unverified Providers |
|---|---|---|
| Product Certification | Health Canada–approved and CNF-notified | Often lack proper registration or notification |
| Labelling Compliance | Bilingual (English/French) with INCI ingredient lists | May have spelling errors, missing ingredients, or English-only labels |
| Educational Support | Training guides on regulatory adherence and best practices | Little to no guidance on compliance requirements |
| Safety Assurance | Adheres to Cosmetic Ingredient Hotlist standards | Risk of containing prohibited or restricted substances |
| Legal Risk | Audit-ready documentation and full traceability | High risk of fines, product recalls, and customs delays |
Pros and Cons of Compliance vs Non-Compliance
Choosing compliance isn’t just a box to tick - it’s a safeguard for your business, your clients, and your professional reputation. Clinics that follow regulations enjoy the benefits of standardized safety protocols, valid liability insurance, and access to Health Canada-approved products. This approach ensures smoother operations, thanks to meticulous record-keeping and the ability to handle adverse events efficiently. On the flip side, non-compliant clinics often face disorganised responses to complications, voided insurance coverage, and heightened risks of lawsuits or regulatory penalties. Essentially, compliance impacts every aspect of running a clinic.
The difference in reputation is just as striking. Compliant clinics earn trust by being transparent and ensuring informed consent, creating a safe and professional environment for clients. Licensed practitioners show accountability by sticking to proper training and regulations. Non-compliance, however, can lead to poor reviews, public disciplinary actions, and a tarnished reputation - especially as clients become more aware of industry standards.
Sourcing is another critical area. Compliant clinics rely on accredited distributors, guaranteeing that all injectables come with a valid Drug Identification Number (DIN) and full traceability. Non-compliant clinics that cut corners by using counterfeit or unauthorised products jeopardize client safety and invite regulatory scrutiny.
The financial risks of non-compliance are also significant. About 30% of complaints against beauty practitioners stem from poor client consent and inadequate documentation. Non-compliance can void liability insurance altogether, leaving practitioners financially exposed if something goes wrong. Tami Blake, a Licensed Esthetician and Founder of Skin + True Skincare, puts it plainly:
"It is not worth losing your license or harming a client over [advanced treatments]. The safest path is always to err on the side of caution and verify with your licensing board."
Here’s a side-by-side comparison of how compliance and non-compliance affect key operational areas:
| Feature | Compliant Clinic | Non-Compliant Clinic |
|---|---|---|
| Operational Efficiency | Standardised protocols, clear delegation, well-organised records | Disorganised management, frequent legal issues, clinic-wide disruptions |
| Reputation | Builds trust with transparency; seen as safe and professional | Damaged reputation from adverse events and public disciplinary actions |
| Sourcing | Uses Health Canada-approved products with valid DINs from trusted distributors | Risks counterfeit or banned products, like hyaluron pens |
| Legal Standing | Protected by liability insurance and adherence to regulations | Exposed to lawsuits, criminal charges, voided insurance, and potential licence loss |
| Patient Safety | Reduces risks and ensures professional handling of complications | Increased chances of infections, scarring, and vascular occlusions |
Conclusion
Meeting compliance standards is the backbone of running a successful beauty clinic in Canada. By using Health Canada-approved products and maintaining valid liability insurance, clinics safeguard their operations at every level. Following federal and provincial regulations not only reduces legal and reputational risks but also fosters trust - an essential factor in attracting and retaining clients.
Clinics that prioritize compliance stand out in the industry. Transparent consent processes, sourcing products with verified Drug Identification Numbers (DINs), and maintaining thorough documentation are key practices that build credibility. These steps protect clinics from issues like counterfeit products, patient harm, and legal challenges, while also giving them a distinct competitive edge.
"Success depends not only on clinical excellence and brand appeal, but on a solid legal foundation that supports professional integrity, regulatory compliance, and commercial viability." - Willis Business Law
The risks of non-compliance are steep. With 30% of complaints against beauty practitioners linked to poor documentation and inadequate consent, the consequences can be both financial and reputational. Working with accredited distributors ensures your clinic operates within the law while providing safe and effective treatments using medical-grade supplies.
Compliance is competence. By adhering to regulatory standards, you’re not just avoiding penalties - you’re building a resilient business that earns client trust, ensures smooth operations, and positions your clinic as a leader in Canada’s aesthetic medicine landscape. Choosing compliance over shortcuts is about safeguarding your patients, your practice, and your professional reputation.
FAQs
How can I quickly confirm a product is Health Canada compliant?
To ensure a product meets Health Canada’s compliance standards, it must be registered or notified with Health Canada. It should adhere to the Food and Drugs Act and Cosmetic Regulations, with accurate ingredient listings and proper labelling. Verification typically involves submitting a Cosmetic Notification Form (CNF).
What records should a clinic keep to stay audit-ready?
Clinics aiming to stay prepared for audits need to keep thorough records. This includes client consent forms, treatment protocols, staff credentials, and documentation of procedures performed. Such records play a key role in showing compliance with regulatory requirements and help ensure audits go smoothly.
Who is legally allowed to inject neurotoxins or fillers in my province?
In Canada, the administration of neurotoxins or fillers is legally restricted to licensed physicians, registered nurses, dentists, and pharmacists. However, the required training and the scope of practice can differ depending on the province or territory. To ensure your safety and compliance with local regulations, always confirm the qualifications of your provider.

Leave a comment